- What is MDM in Healthcare?
- EHR vs. MDM for Healthcare: What’s the Difference?
- What Is the Need for MDM in Healthcare?
- Benefits of Healthcare Master Data Management
- Competitive Advantages of Implementing Healthcare MDM
- Key Components of Healthcare MDM
- Case Study: How MDM Empowered a Leading Healthcare System
- 7 Healthcare MDM Best Practices
- Profisee Master Data Management for Healthcare Is the Optimal Approach for Provider Data
Key Takeaways
Master data management (MDM) in healthcare centralizes and standardizes provider, patient, payor and facility data to improve accuracy and decision making.
Healthcare organizations use MDM to eliminate data silos across HER, HR tools, billing systems and more.
Implementing healthcare MDM successfully requires starting with high-impact domains, aligning cross-functional stakeholders, enforcing strong data governance continuously monitoring data quality.
Profisee MDM for healthcare reduces costs, improves care coordination and helps you meet regulatory demands.
Updated March 13, 2026
Health systems, providers, payers, managed care organizations, telehealth services, critical access hospitals, rural healthcare organizations, accountable care organizations, healthcare exchanges and more all face a common challenge — managing their provider data to offer the most timely and highest quality data.
Data quality may sound like an abstract issue relegated to the IT department, but the truth is, poor healthcare data quality can lead to negative patient experiences. For instance, a study published in Health Affairs reported 53% of patients found inaccuracies in provider data when using health-plan directories to find in-network providers for mental healthcare. In addition to unexpected medical bills, this can lead to patients discovering a provider they believed to be in-network is, in fact, not.
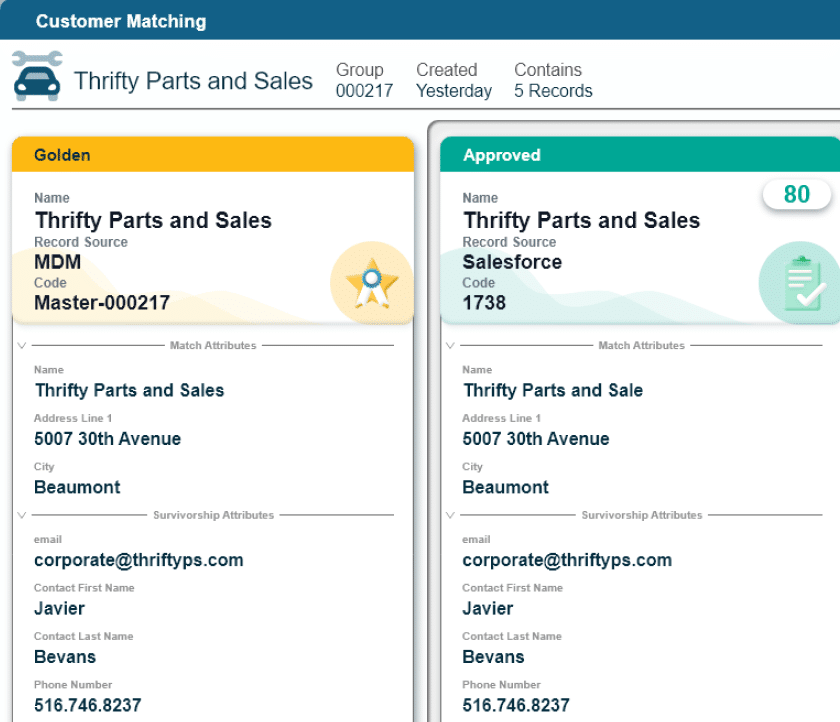
Master data management in healthcare addresses this challenge by creating a unified source of provider data that represents the most accurate, complete, up-to-date and trustworthy information so that patients can find the in-network care they need.
What is MDM in Healthcare?
MDM, or master data management, in healthcare is the process of creating, standardizing and governing key data to keep it accurate, consistent and usable across all systems. Examples of managed master data include patient records, provider credentials, facility details and medical codes.
MDM in healthcare organizations unifies the various systems organizations use, including EHR, HRIS, billing software, supply chain platforms and more. By consolidating the data into a single repository, MDM creates a centralized source of clean, trusted data that helps improve patient care, streamline operations and support compliance with regulations like CMS-0057-F.
Read more: What Is Master Data Management?
EHR vs. MDM for Healthcare: What’s the Difference?
An electronic health record system (EHR) manages clinical data for patient care. MDM, on the other hand, centralizes data from across all systems to keep it clean, consistent and connected. They aren’t a replacement for each other and work best together.
| Feature | Electronic Health Record (EHR) | Master Data Management (MDM) |
|---|---|---|
| Primary Purpose | Stores and manages clinical patient records | Unifies, cleanses and governs shared data across systems |
| Data Type Managed | Diagnoses, treatments, test results, visit history | Patient identities, provider credentials, facility and reference data |
| Scope | One system (clinical workflows) | Multiple systems (EHR, billing, HRIS, supply chain, CRM) |
| Users | Clinicians, nurses, care teams | Data stewards, IT teams, operations, compliance |
| Key Benefit | Improves care delivery and documentation | Ensures data consistency, accuracy and interoperability |
What Is the Need for MDM in Healthcare?
Healthcare organizations are under increasing pressure to manage growing volumes of data while meeting operational and regulatory demands. Master data management in healthcare helps solve the following five challenges:
- Operational efficiency: Healthcare providers are expected to deliver consistent patient care with faster turnaround times while improving data entry standards.
- Data standardization compliance: New regulations require up-to-date, standardized reporting on admissions, discharges and transfers (ADT). Disparate systems make it hard to meet these evolving standards without unified data.
- Healthcare data integration post-M&A: Mergers and acquisitions introduce multiple systems, data formats and workflows. Not only does this strenuous process often take years to accomplish, but it also requires organizations to develop numerous workflows as growth continues.
- Disparate reporting systems: With clinical, billing, HR and supply chain platforms spread across the organization, it becomes difficult to access accurate, consistent information in real time.
- Lack of a single source of truth: Without centralized data, organizations struggle to deliver accurate reporting, coordinate care and ensure system-wide data integrity.
Benefits of Healthcare Master Data Management
Managing provider data through a centralized master data management system delivers measurable value across healthcare operations. From cost control to compliance, MDM helps healthcare organizations maintain accurate, consistent provider records, powering both front-line care and back-office efficiency.
Many organizations begin their MDM journey with provider data management, as it directly supports patient care, compliance and operational efficiency. Provider data is often the most in-demand domain, serving as a single source of truth across clinical, operational and marketing systems. Nine benefits of healthcare master data management include:
- Cost savings: Reduce manual data entry, eliminate duplicate records and cut administrative overhead by maintaining a single source of truth for patient information.
- Improved data quality: Streamline provider credentials, specialties, affiliations and access roles across systems, minimizing mismatches and data fragmentation.
- Regulatory compliance: Avoid fines and audit risks by ensuring accurate provider records that meet federal, state and accreditation requirements.
- Faster provider onboarding: Automate access provisioning for clinical tools and services, accelerating time to productivity for new providers.
- Support for value-based care initiatives: Accurately manage provider participation in Accountable Care Services and shared savings programs.
- Reliable reporting and analytics: Feed clean, standardized provider data into data warehouses and data lakes for accurate, enterprise-wide insights.
- Accurate internal and external directories: Power clinical directories and public-facing provider finders with trusted data, while reducing update and maintenance costs.
- Data interoperability and HIE readiness: Enable compliance with federal interoperability mandates and simplify participation in Healthcare Information Exchanges (HIEs).
- Smarter workforce planning: Identify gaps in physician coverage and support strategic recruitment planning based on accurate, consolidated provider data.
Competitive Advantages of Implementing Healthcare MDM
Leading healthcare organizations continue to implement MDM to improve their data strategy and care delivery, getting a full-spectrum view of their provider and patient data with a way to manage all their critical health information centrally. And leveraging a multidomain MDM platform gives you the flexibility to manage your providers, members/patients and payors within a single platform.
Competitive advantages of healthcare MDM include:
- Improvement in data visibility across domains: Gain a full-spectrum view of provider, patient and payor data to support care coordination, billing and reporting.
- Reduction in operational costs: Eliminate duplicate records, reduce manual reconciliation and streamline data management workflows.
- Enablement of data-driven performance: Use accurate, consistent data to measure outcomes, optimize processes and track KPIs across the organization.
- Acceleration in regulatory compliance: Respond faster to regulatory requirements with standardized data and auditable governance controls.
- Support predictive analytics and AI initiatives: Feed clean, consolidated data into analytics platforms to power population health models, forecasting and strategic planning. By predicting gaps in clinical care with MDM, healthcare organizations can find opportunities for improvement within their network while also expanding access to care for vulnerable populations.
Key Components of Healthcare MDM
A successful healthcare master data management (MDM) strategy depends on the right architectural components working together to manage, standardize and govern data at scale. Here are the key components of any effective healthcare MDM solution:
1. Master Data Domains
Master data management in healthcare covers critical domains such as:
- Provider data: Credentials, specialties, affiliations
- Patient/member data: Identities, contact info, demographics
- Payor data: Insurance plans, coverage details
- Facility data: Locations, certifications, services offered
- Reference data: Medical codes, departments, specialties
2. Data Integration and Ingestion
MDM must connect with multiple source systems, including EHR, CRM, HR platforms, ERP and data lakes. It ingests structured and semi-structured data to create a unified data layer across the organization.
3. Data Matching and Entity Resolution
A core capability of MDM is entity resolution, using algorithms and rules to match, merge and de-duplicate records, ensuring a single, accurate version of each entity.
4. Data Quality Management
MDM includes tools to clean, standardize, validate and enrich data. This component includes address matching and verification, format normalization and rule-based error detection to ensure data is trustworthy and analytics-ready.
5. Data Governance and Stewardship
Robust healthcare MDM systems support role-based access, audit trails and approval workflows, ensuring data changes are governed and traceable. Data stewards play a key role in overseeing quality and enforcing rules.
6. Interoperability and API access
Modern healthcare MDM platforms provide APIs and data services to feed clean master data into downstream systems, supporting real-time updates, regulatory reporting and interoperability initiatives like CMS-0057-F.
Case Study: How MDM Empowered a Leading Healthcare System
A major US healthcare system used Profisee MDM to solve a critical data challenge: provider information was scattered across 50+ credentialing systems, EMR systems and internal data sources. With over 25,000 active providers, the organization needed a centralized, accurate view to support onboarding, analytics and operations. Key challenges included:
- Manual reconciliation of provider data slowed down operations
- Inconsistent records blocked predictive modeling and reporting
- No central source of truth for provider specialties, credentials and locations
With Profisee’s healthcare MDM platform, the team built a centralized provider data pipeline that delivers clean, complete data across the enterprise. Results included:
- 98% provider data completeness
- Daily updates feeding downstream systems for operational use
- More than 200 teams and programs now using trusted MDM data
- MDM adopted as a core strategy by executive leadership
7 Healthcare MDM Best Practices
Implementing master data management in healthcare requires a strategic, cross-functional approach to building a reliable data foundation. Follow these best practices to get the most out of your healthcare MDM program:
- Start with high-impact domains: Focus on domains like provider data and patient identities first. These areas drive immediate value by reducing duplicates, improving care coordination and supporting compliance.
- Align stakeholders early: Involve clinical, IT, compliance and operational teams from the start. A successful healthcare master data management initiative requires cross-functional input and long-term alignment.
- Establish strong data governance: Set clear rules for how data is created, validated and updated. Governance frameworks help prevent inconsistencies and maintain compliance across systems.
- Invest in data stewardship solution: Assign ownership to data stewards who can monitor data quality, resolve issues and enforce policies across departments.
- Choose a multidomain MDM platform: Use a flexible platform that supports provider, patient, payor and facility data, all in one place. This ensures scalability as your data needs grow.
- Design for healthcare interoperability: Ensure your MDM system integrates with EHR, CRM, ERP and other key healthcare platforms. This supports CMS interoperability mandates and future-proofs your data ecosystem.
- Monitor data quality continuously: Don’t treat data cleansing as a one-time task. Implement ongoing monitoring, validation rules and automated alerts to keep your master data clean over time.
Profisee Master Data Management for Healthcare Is the Optimal Approach for Provider Data
EHR, HRIS and CRM tools are essential for daily healthcare operations. But they weren’t designed to manage data across the entire healthcare ecosystem. That’s where the real friction lies: siloed patient records, inconsistent provider directories and disconnected data across departments.
Master data management for healthcare, then, becomes the smarter approach for healthcare providers and networks to manage increasingly complex and disparate provider data.
Profisee is an MDM platform with a solution for the healthcare industry that helps you build a single source of truth across providers, patients, facilities and payors, enabling trustworthy data, faster decisions and better outcomes at scale.
Ready to take control of your provider data? Request a demo of Profisee’s healthcare MDM solution.

Brigitte Tebow
Brigitte Tebow is a Principal Consultant and nationally recognized advisor on master data management (MDM) and data governance in U.S. healthcare. With more than 20 years of experience, she has guided health systems, payers, ACOs and government agencies in modernizing how they manage and govern data to improve clinical, operational and financial outcomes. An award-winning instructor and international speaker, she is a trusted advisor to senior healthcare data leaders on data strategy, interoperability and modernization.